Prof Timothy SC Hinks

Contact information
+44 1865 (2)20885
Rachel Russell-Sharp
rachel.russell-sharp@ndm.ox.ac.uk
 https://orcid.org/0000-0003-0699-2373
https://orcid.org/0000-0003-0699-2373
Room 7400A, Level 7 NDM, John Radcliffe Hospital, Headley Way, Oxford, OX3 9DU, UK
Research groups
The Hinks Lab
The Oxford severe asthma MDT and research nurse team
EXTERNAL COLLABORATORS
We collaborate with a number of groups across UK, Europe and worldwide including:
-Sally Cowley, Oxford Stem Cell Institute, Oxford
-Franze Progatzke, Kennedy Institute of Rheumatology, Oxford
-Julian Knight, Centre for Human Genomics, Oxford
-Peter Bradding, NIHR Leicester Respiratory BRC, UK
-Rachel Clifford, NIHR Nottingham Respiratory BRC, UK
-Peter Howarth, NIHR Southampton Respiratory BRC, UK
-Mustafa Abdo, Deutsches Zentrum für Lungenforschung, Germany
-Theodoros Kapellos, Helmholtz Munich, Germany
-Alexandra Corbett, University of Melbourne, Australia
-David Choy, Genentech, USA
Prof Timothy SC Hinks
BMBCh MA (Cantab) MRCP PhD
Wellcome Trust Fellow & Honorary Consultant
- Associate Professor and Wellcome Trust Career Development Fellow, Respiratory Immunology, Nuffield Dept of Medicine
- NIHR Oxford Biomedical Research Centre Senior Research Fellow
- Honorary Consultant, Oxford Special Airway Service, Respiratory Medicine, Oxford University Hospitals NHS Trust
Investigating immune responses in asthma and lung infections
Research Interests
My group investigate the immunopathogenesis of airway diseases and pulmonary infections. We have a specific focus on the roles of unconventional T cells subsets in the mucosal immunology of the airways in driving inflammation during chronic airways infection, and gene expression and epigenomics of specific asthma phenotypes.
After a background in translational research in T cell immunodiagnostics in tuberculosis I have been funded by fellowships from the Wellcome Trust, Academy of Medical Sciences and National Institute of Health Research to study novel T cell subsets in the airways in human asthma and more recently the roles of mucosal associated invariant T (MAIT) cells in ex vivo and murine models of infection with Haemophilus influenzae, Legionella and Influenza virus. Our recent work has defined novel functions for MAIT cells in tissue repair, identified mechanisms of macrolides in airways diseases and generated a new two-compartment model of asthma pathology.
Our goal is to apply single cell, spatial and classical immunological approaches to better understand the immunopathogenesis of asthma, to help develop new therapies.
Funding

Research groups
Innate T cells in airways disease
Pulmonary spatial transcriptomics
Websites
-
Volunteer as a research participant
If you would be interested in volunteering in our research studies, either as a healthy control or as someone with asthma, fill in this form and we can tell you more
-
Our research bronchoscopies
Find out what its like to volunteer for one of our research bronchoscopy studies
-
Bronchoscopies explained
The full length video - watch research volunteer Tom undergo a bronschoscopy
-
Severely asthma - Peter's story
Listen to Peter's experience of living with severe asthma, and the transformative effects of new treatments
Recent publications
Treatable traits and treatment options in asthma.
Journal article
Kanabar SS. et al, (2026), Respiratory medicine
Fractional exhaled nitric oxide and the response to prednisolone for asthma attacks in patients treated with anti-IL5/5Rα therapy: a prospective observational study
Journal article
Howell I. et al, (2025), European Respiratory Journal, 66, 2501229 - 2501229
Protective Role for Itaconate During Inhaled Allergen Challenge.
Journal article
Albers GJ. et al, (2025), Allergy
Inflammatory and clinical risk factors for asthma attacks (ORACLE2): a patient-level meta-analysis of control groups of 22 randomised trials.
Journal article
Meulmeester FL. et al, (2025), The Lancet. Respiratory medicine, 13, 505 - 516


 ©
Hinks Lab, 2023
©
Hinks Lab, 2023
 ©
OUH Trust 2023
©
OUH Trust 2023
 ©
Image c/o Maisha Jabeen, Hinks Lab
©
Image c/o Maisha Jabeen, Hinks Lab
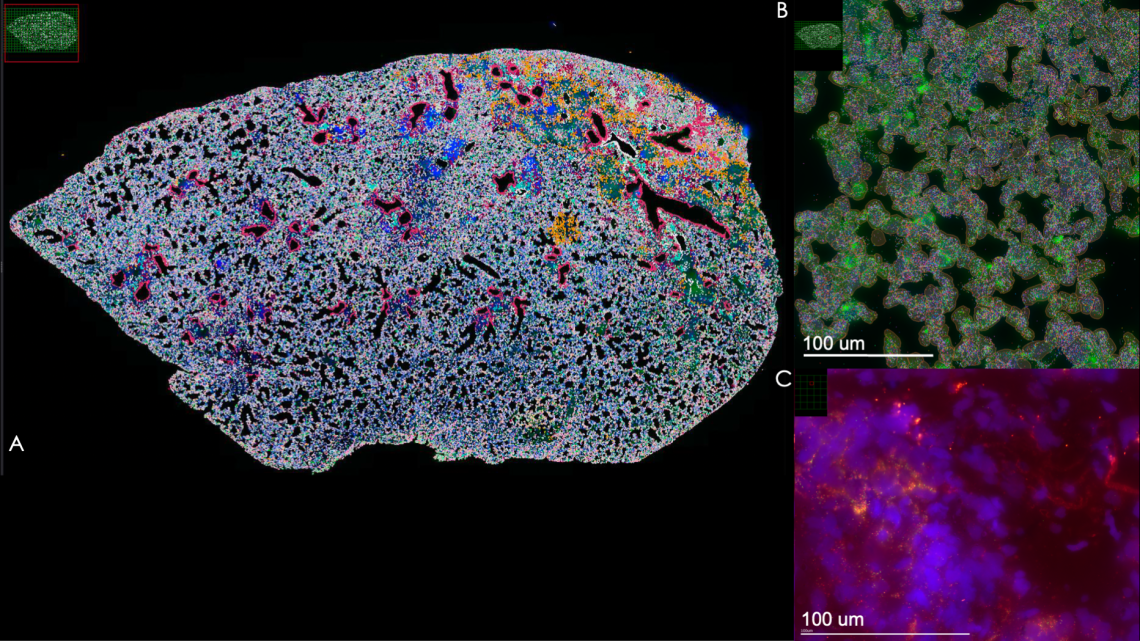 ©
Image c/o Xiawei Zhang, James Melhorn, Hinks Lab
©
Image c/o Xiawei Zhang, James Melhorn, Hinks Lab