Professor Wirichada Pan-ngum

Contact information
Research groups
Podcast interview
Modeling for maximum impact on health research
Wirichada leads a modelling group using statistical and mathematical approaches to address regional health challenges. Her work on hepatitis C informed Thailand’s treatment and screening policies. Current priorities include integrating AI into modelling and addressing climate change and mental health. Her team also focuses on local capacity building for sustainable impact.
Wirichada Pan-ngum
Associate Professor
- Honorary Visiting Research Fellow
- Acting Head of MAEMOD
MAEMOD
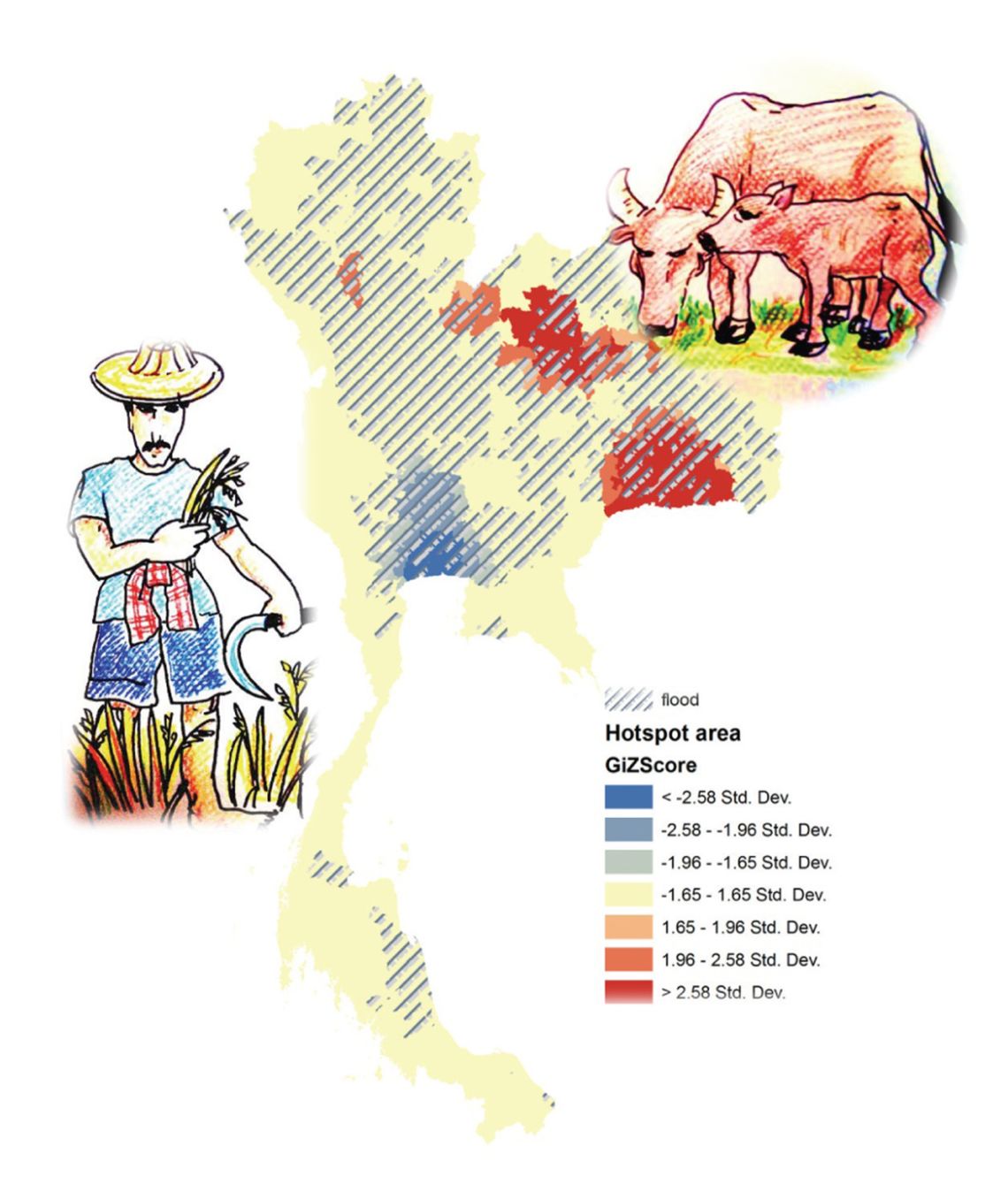
Wirichada Pan-Ngum’s research mainly involves using a mixed approach including modelling and field surveys to gain better understanding of transmission routes of zoonotic diseases and the Human-Animal-Ecosystems interface. Her current work focuses on leptospirosis, one of many long-term health problems for agricultural workers in Thailand. Her model explores the importance of these environmental factors as well as the risk of disease exposure during traditional rice farming activities in relation to the incidence of human leptospirosis. Her other research interests include dengue, human contact patterns and population dynamics for infectious disease modelling.
In addition to her work at MORU, Wirichada is an Associate Professor in the Department of Tropical Hygiene, Faculty of Tropical Medicine at Mahidol University. She teaches biostatistics and mathematical modelling. In addition, she serves as a project advisor for postgraduates on the Tropical Medicine and Biomedical and Health Informatics courses.
Recent publications
Economic evaluation of biomarker-based surveillance for Hepatocellular Carcinoma in Thai patients with Compensated Liver Cirrhosis.
Conference paper
Pinjaroen N. et al, (2026), PloS one, 21
Mathematical modeling of control strategies for the elimination of soil-transmitted helminthiases in Thailand.
Journal article
Chuaicharoen P. et al, (2025), PLoS neglected tropical diseases, 19
Enhancing global health security responses through greater inclusion of the global south in infectious disease modelling.
Journal article
Leung K. et al, (2025), BMJ global health, 10
Optimizing dog population control strategies in Thailand using mathematical and economic modeling.
Journal article
Thichumpa W. et al, (2025), PLoS neglected tropical diseases, 19
Factors Influencing Health Workers' Acceptance of Guideline-Based Clinical Decision Support Systems for Preventive Services in Thailand: Questionnaire-Based Study.
Journal article
Sitasuwan T. et al, (2025), JMIR human factors, 12